Racial and Ethnic Medicare Disparities and COVID-19
United Church of Christ – Wider Church Ministries
Humanitarian Development Team
Coronavirus (COVID-19) Daily Briefing
Barbara T. Baylor, MPH – Temporary Health Liaison
Racial and Ethnic Medicare Disparities and COVID-19
“No longer will older Americans be denied the healing miracle of modern medicine. No longer will illness crush and destroy the savings that they have so carefully put away over a lifetime so that they might enjoy dignity in their later years.”
– U.S. President Lyndon Johnson in July 1965,
signing Medicare and Medicaid into law.
In 1965, then President Lyndon Johnson signed the Older Americans Act and formally declared May as Older Americans Month. The Act addressed the growing concerns of America’s then 17 million individuals aged 65 and older.
At the time, one-third of all seniors lived in poverty, with few social programs available to help support them. The Older Americans Act introduced nutrition programs, transportation assistance, federally funded adult day care, legal assistance and other services for seniors.
Significantly, it also paved the way to creation in July 1965 of Medicare and Medicaid, which offer healthcare insurance to seniors.
Today, as the primary source of health insurance coverage for people aged 65 years and older, Medicare is instrumental in ensuring access to affordable health coverage. Traditional Medicare currently covers roughly 33 million older adults, and about 18 million more are covered under Medicare Advantage (MA), the program’s private plan option.
As the nation’s largest purchaser and regulator of healthcare, Medicare plays an important role in expanding coverage, improving the affordability of healthcare for vulnerable populations, and reducing racial and ethnic disparities in health coverage and access to care.
 But while the program has a positive track record of reducing disparities based on race and ethnicity, disparities persist even within the Medicare population – in access, service use and health outcomes, with Blacks and Hispanics experiencing worse health indicators and receiving lower quality of care than Whites.
But while the program has a positive track record of reducing disparities based on race and ethnicity, disparities persist even within the Medicare population – in access, service use and health outcomes, with Blacks and Hispanics experiencing worse health indicators and receiving lower quality of care than Whites.
Furthermore, within Medicare Advantage plans, a recent study found that beneficiaries in racial and ethnic minority groups reported experiences with healthcare that were worse than or similar to the experiences reported by white beneficiaries.
These disparities mirror the inequities in health coverage and care that exist generally in the United States.
What’s going on here? One important factor is the ability or inability to pay for supplementary healthcare insurance to cover the 20 percent of costs not covered by traditional Medicare.
An AARP policy analysis shows that older Blacks and Hispanics with traditional Medicare are significantly less likely to have supplemental coverage (Medigap, Medicaid or retiree health insurance) than Whites, contributing to less use of physician services and, consequently, poorer health.
Older Blacks and Hispanics are generally less able to afford the cost of a Medigap plan than Whites. Median income is significantly higher for White Medicare beneficiaries ($30,050) than for Blacks ($17,350) and Hispanics ($13,650). In addition, lower levels of access to retiree health insurance among Blacks and Hispanics also contribute to disparities in supplemental insurance coverage.
Specifically in the COVID-19 pandemic, for the roughly one-third of Medicare beneficiaries enrolled in Medicare Advantage, large insurers have voluntarily waived out-of-pocket costs for COVID-19 treatment. Most older adults with traditional Medicare will not have to pay the program’s $1,408 deductible (called the Part A deductible) associated with an inpatient hospital stay.
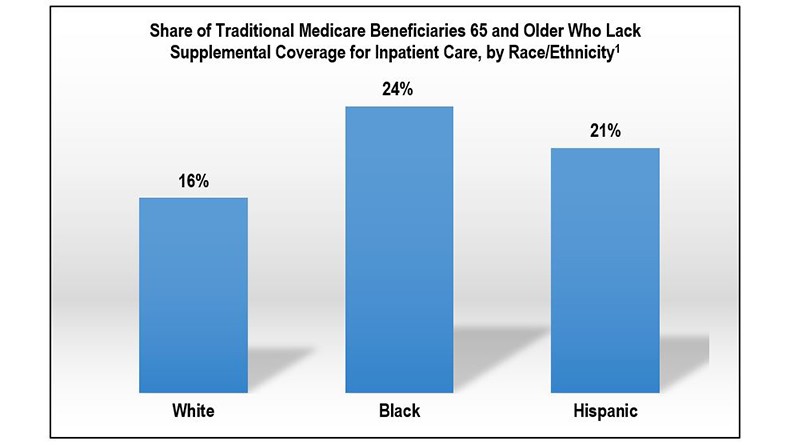
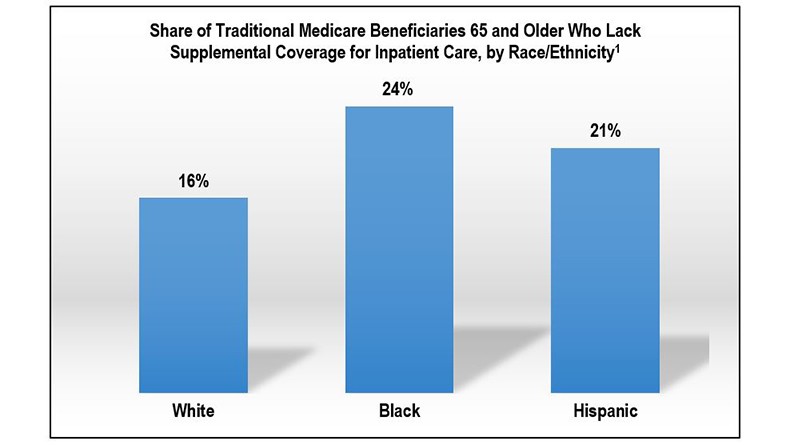
But 5 million people with traditional Medicare would be at risk for high out-of-pocket costs related to COVID-19 hospital treatment, including one in four (24 percent) of Blacks and one in five (21 percent) of Hispanics compared to one in six (16 percent) of Whites.
This is on top of disproportionately high rates of severe illness or death for older adults, with Blacks and Hispanics even more disproportionately affected: 30 percent of COVID-19 patients are African American even though they make up 13 percent of the U.S. population (17/29.6 percent for Hispanics).
These multiple disparities underscore a need for policymakers to ensure that all Medicare beneficiaries have protection from burdensome out-of-pocket spending for COVID-19 treatment.
Congress recently mandated free COVID-19 testing for all Medicare beneficiaries. But what happens once someone gets a positive result back and needs COVID-19 treatment? What is needed is for Federal policymakers to put in place cost protections for all Medicare beneficiaries. Cost protections would help ensure that people will not face a deductible and other cost-sharing for COVID-19 treatment and allow them to focus on their recovery rather than worry about how they will pay their medical bills.
The impact of COVID-19 has highlighted where significant disparities and needs still exist when it comes to the health of older adults, especially racial and ethnic older adults. As Older American Month draws to a close, hard truths remain about how far we still must go to ensure the health and well-being of older adults in our community. Improving access to affordable, high-quality health coverage and care for all Americans remains one of the nation’s formidable policy challenges.
1) AARP Graphic
Related News
Planning for Earth Month: Resources for Congregations
April is Earth Month, and for congregations, it can be a great time to further discern how...
Read MoreGrowing Weary
In December 1964 during a speech in Harlem, Fannie Lou Hamer declared: “And you can always...
Read MoreBodily Autonomy Means Every-BODY
Advocacy and Action for Women's and Gender Justice Local events stir thoughts and...
Read More